
3R-INFO-BULLETIN 25
| | January 2003The Authors  
The model was developed in the Research group on Vascular Biology headed by Professor Dr. E. Battegay (left). The experimental part was coordinated by Dr. R. Humar (middle). The portion of the present study dealing with rodent heart pieces was carried out by Dr. F. Kiefer (right) in the framework of his PhD-thesis.
Current addresses: Edouard Battegay
ebattegay@uhbs.ch
Medical Outpatient Department
University Hospital Basel
Petersgraben 4
CH-4031 Basel
Switzerland Rok Humar and Fabrice Kiefer
rok.humar@unibas.ch, fabrice.kiefer@unibas.ch
Division of Vascular Biology
Department of Research
University Hospital Basel
Petersgraben 4
CH-4031 Basel
Switzerland
Editor
Peter Maier, Scientific Adviser of the 3R Research Foundation |
Formation of new blood vessels in the heart can be studied in cell cultures
Current in vivo models in angiogenesis research often results in painful conditions for the animals. The aim of the present successful project (Nr. 76-01, supported by the 3R Research Foundation, Switzerland), was to adapt an in vitro assay used in aorta angiogenesis specifically to study angiogenesis in the heart of mammals. Such an approach might replace a significant part of widely performed animal experiments in the area of therapeutic angiogenesis.
Formation of new blood vessels, a therapeutic concept
Coronary heart disease is very common in human. It often causes hypoxia and myocardial ischemia as one of the severe consequences. This affects the function of the heart and results in a significant morbidity and mortality for the patient. Stimulation of angiogenesis (development of new blood vessels) by pharmacological or molecular methods (therapeutic angiogenesis)[*] would generate the formation of new coronary collaterals in the myocardium, i.e., small branches of arteries and veins that develop to bypass narrowed or blocked segments. Improving coronary collateral circulation would limit myocardial ischemia and is therefore a promising new concept (1).
Three-Dimensional cell cultures
Models of angiogenesis in vitro are based on the capacity of activated endothelial cells (cells forming the walls of blood vessels) to invade three-dimensional substrates. These substrates (Matrix) may consist of collagen gels, plasma clot, purified fibrin, Matrigel, or a mixture of these proteins with others. It is possible to embed and culture pieces of blood vessels (vascular explants such as aortic rings) and to observe cells sprouting and forming capillary-like structures (CLS) (3). These models allow the preservation of the vessel architecture during the in vitro assay, and thus are close to an "ex vivo" model (4). One particular model of angiogenesis (the Nicosia-model), used for in vitro angiogenesis of aortic explants, was further developed for heart explants. Briefly, pieces (ca. 1 mm3) of left ventricular myocardium of rat or mouse hearts are embedded in a fibrin-gel, overlayed with growth medium and angiogenic stimulants (agonists) and/or inhibitors (antagonist). These cultures are then incubated for 10 days. Active molecules are added again every third day, and oxygen saturation can be lowered down to 1% O2 (Fig. 1). A single mouse heart allows to assess more than 20 different samples, each tested in octuplicates.
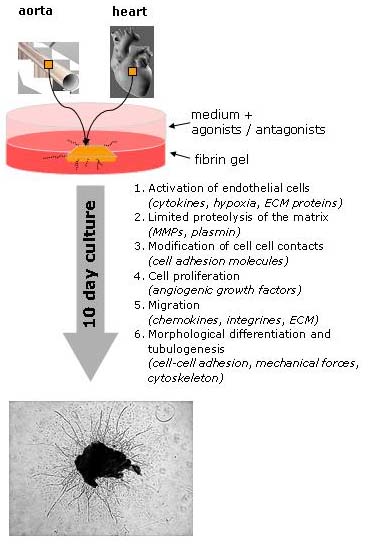 Fig. 1: Schematic represenation of three-dimensional angiogenesis assay in vitro; heart and aorta explants embedded in gel give rise to capillary sprouts (CLS).
Fig. 1: Schematic represenation of three-dimensional angiogenesis assay in vitro; heart and aorta explants embedded in gel give rise to capillary sprouts (CLS).
Reproducibility of the in vitro system
First we tested basic culture conditions to ensure reproducibility of the assay. In contrast to aortic explants forming CLS in serum-free conditions, CLS formation of heart explants requires fetal calf serum (FCS, 5%) to ensure survival, whereas too high FCS concentrations mask the activity of angiogenically active molecules. In heart explants from mice younger than 8 weeks, CLS formed spontaneously-an unwanted response for testing the stimuli of angiogenic active factors. In 12-week-old adult mice however, virtually no CLS was formed under normoxia (standard culture condition, 19% O2). Sex of the animals did not account for differences observed in CLS formation. Thus, for our future experiments, we chose adult mice, older than 12 weeks, to abolish the effect of active angiogenesis during adolescence of animals. Under hypoxia (3% O2) however, CLS formation substantially increased, an established feature of angiogenesis, observed in vivo and in vitro.
Differential response toward angiogenic factors
Different classic angiogenic molecules induced diverse CLS: Platelet Derived Growth Factor (PDGF-BB) induced outgrowth of a mixture of organized branched endothelial sprouts, unorganized single endothelial cells and pericytes/smooth muscle cells. In contrast, basic Fibroblast Growth Factor (beta FGF) induced mainly unbranched, elongated CLS. Vascular Endothelial Growth Factor (VEGF165) induced elongated CLS, and branching appeared complex (Fig. 2).
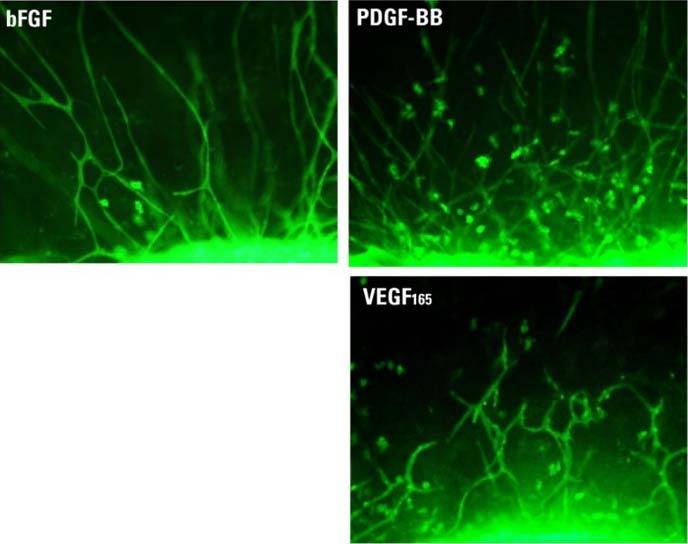
Fig. 2: Differential morphology of CLS can be observed after administration of different angiogenic molecules to mouse heart explants: basic Fibroblast Growth Factor - beta FGF (10 ng/ml), Platelet-Derived Growth Factor B-dimer -PDGF-BB (10 ng/ml), Vascular Endothelial Growth Factor - VEGF (5 ng/ml).
In vivo like response
Independent of the morphology induced by different agonists, outgrowing sprouts were composed of endothelial cells by more than 90% when outgrowing cells were subcultured and assessed by endothelial cell marker CD31, Dil-Ac-LDL. Double in-gel-staining with FITC-coupled lectin G. simplicifolia (green fluorescent) and Cy3-coupled antibody against -smooth muscle actin (red fluorescence) revealed endothelial sprouts with single attached smooth muscle cell-like cells (pericytes) (Fig. 3). Pericyte attachment forming endothelial tubes have been observed in vivo and contributes to vessel remodeling, maturation and stabilization.
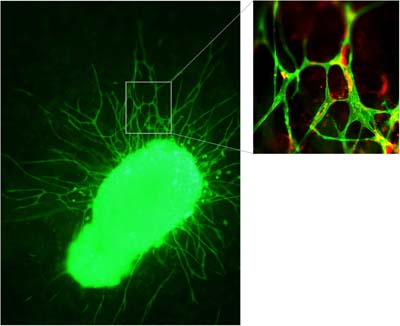
Fig. 3: In-gel characterization of CLS by FITC-coupled lectin G. simplicifolia (green fluorescent) and Cy3-coupled anti alpha-smooth muscle actin-staining (red staining).
Organ specific response
Mechanisms involved in angiogenesis of the heart were further investigated in explants derived form transgenic mice lacking genes involved in angiogenesis. As an example, the role of nitric oxide (NO) in angiogenesis: NO promotes not only blood vessel relaxation and regulates vascular tone, but is critical for angiogenesis initiation and modulation (5). We investigated the role of inducible nitric oxide synthase (iNOS) under conditions of moderate hypoxia (3% O2). In heart explants from iNOS (-/-) mice no CLS could be formed, regardless of angiogenic stimuli used (Fig. 4), whereas in aortae explants CLS was reproducibly formed from, however, at a reduced level when compared to wild type aorta (Fig. 4). Thus, iNOS requirement for angiogenesis is organ specific, optional for the aorta, but mandatory for the heart.
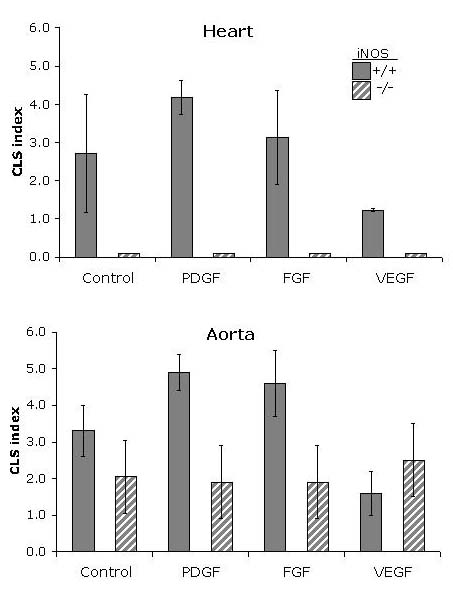 Fig. 4: Role of iNOS in angiogenesis: In vitro angiogenesis of aorta and heart in iNOS (-/-) mice under hypoxia (3% O2). A standardized scale ranging from 0 to 8 indicated the degree of sprouting (CLS index). In aortae of iNOS (-/-) mice, in vitro angiogenesis in response to beta FGF, VEGF and PDGF-BB is present but strongly reduced when compared to wild type (+/+) animals. In hearts of iNOS (-/-) mice, angiogenesis was completely abrogated conditions when compared to wild-type animals.
Fig. 4: Role of iNOS in angiogenesis: In vitro angiogenesis of aorta and heart in iNOS (-/-) mice under hypoxia (3% O2). A standardized scale ranging from 0 to 8 indicated the degree of sprouting (CLS index). In aortae of iNOS (-/-) mice, in vitro angiogenesis in response to beta FGF, VEGF and PDGF-BB is present but strongly reduced when compared to wild type (+/+) animals. In hearts of iNOS (-/-) mice, angiogenesis was completely abrogated conditions when compared to wild-type animals.
A versatile in vitro model
The present in vitro angiogenesis model (6) of the heart allows:
- assessing angiogenesis in mouse and rat hearts. Both, induction and repression of angiogenesis can be investigated.
- rapid screening of pharmacological compounds by using only a small number of animals.
- different type of angiogenical active stimuli to be investigated due to the flexibility of experimental conditions.
- the use of tissue from knockout mice to investigate the role of specific genes in heart angiogenesis.
Together, a wide range of questions connected with therapeutic angiogenesis can be answered without the use of in vivo experiments.
Published updated version of this Bulletin 25/2007 (PDF)
References:
- Freedman SB, Isner JM. Therapeutic angiogenesis for coronary artery disease. Ann Intern Med. 2002;136:54-71.
- Schumacher B, Pecher P, von Specht BU, Stegmann T. Induction of neoangiogenesis in ischemic myocardium by human growth factors: first clinical results of a new treatment of coronary heart disease. Circulation. 1998;97:645-50.
- Nicosia RF, Ottinetti A. Growth of microvessels in serum-free matrix culture of rat aorta. A quantitative assay of angiogenesis in vitro. Lab Invest. 1990;63:115-22.
- Vailhe B, Vittet D, Feige JJ. In vitro models of vasculogenesis and angiogenesis. Lab Invest. 2001;81:439-52.
- Sieber CC, Sumanovski LT, Stumm M, van der Kooij M, Battegay E. In vivo angiogenesis in normal and portal hypertensive rats: role of basic fibroblast growth factor and nitric oxide. J Hepatol. 2001;34:644-50.
- Kiefer F, Munk V, Dieterle T, Humar R, Battegay EJ. A versatile model of angiogenesis in the rodent heart. In revision.
| [*] | Animal models for the development of new therapeutic conceptsAngiogenesis is a process of creating new arteries, veins and capillaries in order to increase the blood supply within an organ or tissue. It occurs for example in response to signals from an organ or tissue that is insufficiently oxygenated. In the heart, angiogenesis occurs in response to acute or chronic blockages (occlusions) of coronary arteries. These occlusions induce a state of hypoxia known as myocardial ischemia. Patients with coronary heart disease often have a better clinical outcome if angiogenesis can be stimulated (therapeutic angiogenesis) and the collateral blood circulation within the heart can be improved. Accordingly, substantial research resources are currently being invested into studying the therapeutic stimulation of angiogenesis. Multiple animal studies and some preliminary human studies have confirmed the concept of stimulation of collateral circulation by pharmacological or molecular methods (2). Current animal models of angiogenesis in vivo often use complete blockage by ligation or a gradual reduction of blood flow in a major coronary artery to induce hypoxia-driven angiogenesis. Many animals die due to myocardial infarction or cardiac rhythm disturbances during these sometimes cumbersome surgical procedures. Furthermore, myocardial ischemia is often quite a painful condition for the animals. |




 Fig. 1: Schematic represenation of three-dimensional angiogenesis assay in vitro; heart and aorta explants embedded in gel give rise to capillary sprouts (CLS).
Fig. 1: Schematic represenation of three-dimensional angiogenesis assay in vitro; heart and aorta explants embedded in gel give rise to capillary sprouts (CLS).

 Fig. 4: Role of iNOS in angiogenesis: In vitro angiogenesis of aorta and heart in iNOS (-/-) mice under hypoxia (3% O2). A standardized scale ranging from 0 to 8 indicated the degree of sprouting (CLS index). In aortae of iNOS (-/-) mice, in vitro angiogenesis in response to beta FGF, VEGF and PDGF-BB is present but strongly reduced when compared to wild type (+/+) animals. In hearts of iNOS (-/-) mice, angiogenesis was completely abrogated conditions when compared to wild-type animals.
Fig. 4: Role of iNOS in angiogenesis: In vitro angiogenesis of aorta and heart in iNOS (-/-) mice under hypoxia (3% O2). A standardized scale ranging from 0 to 8 indicated the degree of sprouting (CLS index). In aortae of iNOS (-/-) mice, in vitro angiogenesis in response to beta FGF, VEGF and PDGF-BB is present but strongly reduced when compared to wild type (+/+) animals. In hearts of iNOS (-/-) mice, angiogenesis was completely abrogated conditions when compared to wild-type animals.