
3R-Project 81-02
In vitro model for the testing of endothelial cell activation and damage in whole blood
Yara Banz and Robert Rieben
Department of Clinical Research, Cardiovascular Research, 3010 Bern, Switzerland
robert.rieben@dkf.unibe.ch
Keywords: human; pig; whole blood; endothelia; coagulation; complement system; transplantation; microcarrier; reduction; replacement; drug screening
Duration: 2 years Project Completion: 2005
Background and Aim
Acute damage and activation of endothelial cells (EC), the inner lining of blood vessels, is encountered in sepsis or septic shock, in ischemia/reperfusion (I/R) injury, and in acute vascular rejection after allo- or xenotransplantation. There is increasing evidence that the complement system is a key player for the induction of EC damage. Ischemia-induced changes on the EC-membrane, or the binding of antibodies in the case of transplantation, lead to activation of the classical complement cascade. The main consequence of this complement-attack is activation of the EC, which means that heparan sulfate proteoglycans are released and a procoagulant cell surface exposed. This leads to activation of the coagulation cascade and, in turn, to more damage and activation of EC. One strategy to prevent EC damage is therefore inhibition of the complement and coagulation cascades. We have been developing soluble complement inhibitors and analyzing their potential role as "EC protectants". Up until recently, the interplay between EC, complement and coagulation in whole blood could only be studied in animal experiments because of the tendency of blood to coagulate spontaneously in vitro. However, a new technique in which EC are cultured on microcarrier beads now allows whole, non-anticoagulated blood to be incubated together with EC. Using this new EC culture system we have:
· establish an in vitro model for EC activation and damage that allows the complex interactions of non-anticoagulated, whole blood with EC, as normally observed in vivo, to be studied in vitro.
· (pre)validate the above model for the study of EC protection by using known "EC protectants", such as low molecular weight dextran sulfate (DXS)
In forthcoming studies we will screen and evaluate the potential of novel, soluble complement inhibitors / "EC protectants" mainly in the context of ischemia/reperfusion injury and transplantation.
Method and Results
1. Establishment of an in vitro model for EC activation and damage
EC damage in vitro has been explored in a pig-to-human xenotransplantation model. For this purpose, porcine aortic EC (PAEC) were cultivated on microcarrier beads to increase the surface-to-volume ratio and incubated with whole, non-anticoagulated human blood as an antibody and complement source. This system functions as a model for (hyper)acute vascular rejection in the setting of xenotransplantation. Immunohistochemistry and immunofluorescence analyses were used to measure activation of both the complement and the coagulation systems, as well as complement deposition on the EC-beads. EC survival was monitored and tests performed to measure the influence of EC damage on activation of the coagulation cascade (see Figure 1 and 2).
2. (Pre)validation of the above model to study EC protection
The known EC protectants dextran sulfate (DXS) was used in the EC activation and damage model and its effect on the different test parameters evaluated. This substance successfully prevented activation of the complement system, and therefore also the activation of EC.
3. Screening of novel, soluble complement inhibitors / "EC protectants"
Our group is currently developing fully synthetic, soluble complement inhibitors / EC protectants that have less systemic side effects on the coagulation system than DXS. These novel substances are currently being screened in both complement and coagulation assays with human plasma. Instead of immediate in vivo application in the hamster-to-rat transplantation model (the current procedure), the in vitro assay for EC protection with whole blood – as developed and validated under 1) and 2) – is being used in a second screening round.
Conclusions and Relevance for 3R
Currently, in most in vitro models in which whole blood or plasma is brought into contact with EC, anticoagulants are required to prevent clotting. This makes it difficult, if not impossible, to analyze in vitro the importance of the coagulation system in EC activation and damage. To date, the possibilities to analyze and screen substances in vitro that could potentially act as "EC protectants" are therefore limited. In consequence, animal models of e.g. I/R injury, transplantation, or shock have to be applied at early stages of scientific research and drug development. In the present project we strive to develop a model of EC activation and damage that can be used to study the interaction of EC with whole, non-anticoagulated blood in vitro. This model is now available and enable us to reduce the need of animal testing and replace part of the currently used in vivo experiments by in vitro screening.
(see also 3R-INFO-BULLETIN Nr. 34)
Published updated Version 34/2007 (pdf)
References
Banz Y., Cung T., Korchagina E.Y., Bovin N.V., Haeberli A. and Rieben R. (2005) Endothelial cell protection and complement inhibition in xenotransplantation: a novel in vitro model using whole blood. Xenotransplantation, 2005 (in press).
Figures
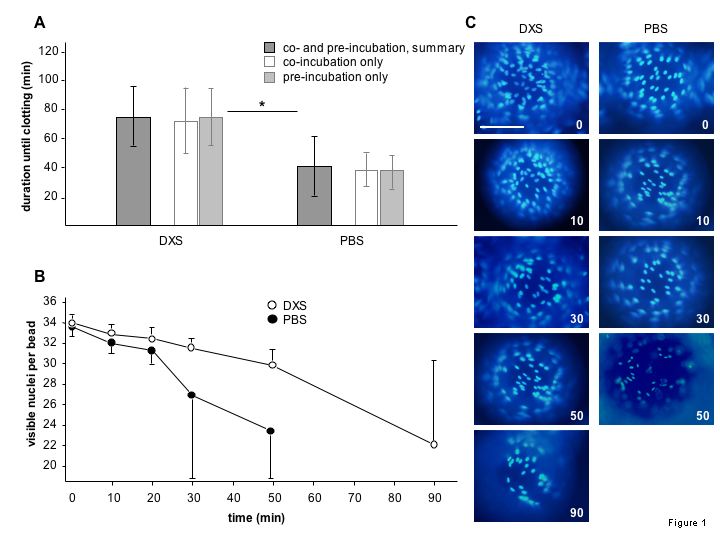
Figure 1: Shown is the duration of the experiments in minutes until occurrence of clotting (A) and the cell-count (porcine aortic endothelial cells) on the bead surface, counted as visible nuclei per bead surface (B). Representative images of single beads at baseline (0 min), after 10, 30, 50 and 90 min of incubation with human blood are shown(C). DAPI staining for nuclei. Scale bar represents 100 µm.
Figure 2
Immunofluorescence staining (A) and grading for expression of von Willebrand Factor with 0 = no positivity, 1 = minimal positivity, 2 = moderately strong positivity, 3 = strong positivity (B). Representative picture of a bead with fluorescein-labeled DXS bound to porcine aortic endothelial cells. Scale bars represent 100 micrometer.
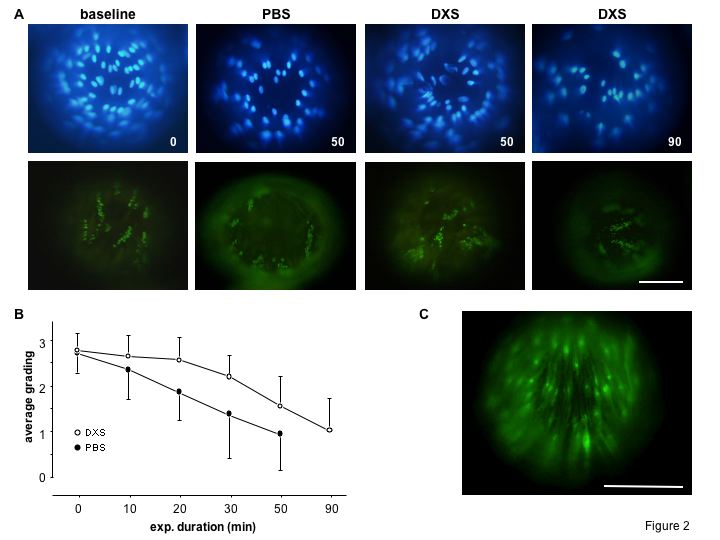
Figure 2


